
Efectividad de una Intervención Psicoeducativa en la Reducción de la Sobrecarga del Cuidador Informal del Paciente con Esquizofrenia (EDUCA-III-OSA)
[Effectiveness of a psychoeducational intervention in reducing burden in informal caregivers of schizophrenic patients (EDUCA-III-OSA)]
Eduardo González-Frailea, María Teresa Bastida-Loinazb, Manuel Martín-Carrascoc, Ana I. Domínguez-Panchónd, Álvaro Iruin-Sanzb y grupo EDUCA-III-OSA
aUniversidad Internacional de La Rioja (UNIR), España; bRed de Salud Mental de Gipuzkoa, Osakidetza, Gipuzkoa, España; cClínica Psiquiátrica Padre Menni, Pamplona, España; dHospital Aita Menni, Arrasate-Mondragón, Guipuzkoa, España
https://doi.org/10.5093/pi2018a20
Recibido a 17 de July de 2018, Aceptado a 12 de March de 2018
Resumen
Los familiares de pacientes con esquizofrenia o trastorno esquizoafectivo frecuentemente padecen consecuencias negativas derivadas de su labor como cuidadores. El objetivo del estudio EDUCA-III-OSA es evaluar la efectividad de un programa de intervención psicoeducativa (PIP) en la reducción de la sobrecarga del cuidador informal tras la intervención a los 4 meses y 16 meses después. Se llevó a cabo un estudio multicéntrico con diseño cuasi-experimental de grupo único. La variable dependiente principal fue la sobrecarga, medida a través del Inventario de Sobrecarga de Zarit (ZBI) y el Cuestionario de Evaluación de Repercusión Familiar (IEQ). Las variables secundarias fueron la ansiedad (STAI-X), la salud mental del cuidador (GHQ-28) y la depresión (CES-D). 39 cuidadores de 5 centros diferentes participaron en el estudio. Tras la intervención (4 meses), las variables de sobrecarga (d de Cohen = 0.26), depresión (d = 0.42), salud mental (d = 0.76) y ansiedad-estado (d = 0.59) experimentaron una mejora moderada. Esta mejora se vio incrementada a los 16 meses en las variables de sobrecarga (d = 0.56) y ansiedad-estado (d = 0.89), mientras que la variable de salud mental experimentó un descenso (d = 0.39). Tras la aplicación de la intervención psicoeducativa manualizada se produjo una mejoría en el estado psicológico de los cuidadores informales. Estos cambios se mantuvieron un año después.
Abstract
Families of patients with schizophrenia usually experience negative consequences. The aim of the EDUCA-III-OSA study is to test the effectiveness of a psychoeducational intervention program (PIP) to reduce the caregiver burden at postintervention (4 months) and at follow-up (16 months). A multicentre quasi-experimental study design with a unique group of informal caregivers who received intervention was used. The intervention consisted of 12 weekly group sessions. The primary outcome variable was burden, measured through the Zarit Burden Interview (ZBI) and the Involvement Evaluation Questionnaire (IEQ). Secondary outcome variables were anxiety (STAI-X), mental health (GHQ-28), and depression (CES-D). 39 caregivers from 5 research sites participated in the study. After the intervention (4 months), the variables of burden (Cohen’s d = 0.26), depression (d = 0.42), mental health (d = 0.76), and anxiety-state (d = 0.59) showed a moderate decrease. These improvements increased 16 months later in the variables of burden (d = 0.56) and anxietystate (d = 0.89), while the mental health variable decreased (d = 0.39). After the application of the intervention program a marked improvement in the psychological status of informal caregivers was produced. These changes held one year later.
Palabras clave
Esquizofrenia, Cuidador, Salud mental, Diseño cuasi-experimental.
Keywords
Schizophrenia, Caregivers, Mental health, Quasi-experimental design.
Para citar este artículo: González-Fraile, E., Bastida-Loinaz, M. T., Martín-Carrasco, M., Domínguez-Panchón, A. I., Iruin-Sanz, A. y grupo EDUCA-III-OSA (2018). Efectividad de una intervención psicoeducativa en la reducción de la sobrecarga del cuidador informal del paciente con esquizofrenia (EDUCA-III-OSA). Psychosocial Intervention, 27, 113-121. https://doi.org/10.5093/pi2018a20
Financiación. El estudio EDUCA-III-OSA ha sido financiado por el Departamento de Salud del Gobierno Vasco.
Correspondencia: eduardo.gonzalez@unir.net (E. González-Fraile).
Introducción La esquizofrenia es una enfermedad mental de larga evolución que produce graves consecuencias tanto en el paciente, como en el cuidador (van Os y Kapur, 2009). La Organización Mundial de la Salud estima que cerca de 21 millones de personas padecen la enfermedad en todo el mundo (Whiteford et al., 2013). La esquizofrenia afecta principalmente al paciente y sus habilidades para llevar a cabo las actividades de la vida diaria, pero también a sus familiares y a la sociedad en general (Caqueo-Urizar et al., 2017; Chong et al., 2016). Dentro de la familia, destaca la figura del cuidador principal como responsable de la atención a la persona afectada. Este cuidador desempeña importantes labores de apoyo hacia el enfermo, ayudándole a afrontar las tareas relacionadas con aspectos socio-económicos (integración social, ocupación, soporte financiero), el soporte emocional y las actividades de la vida diaria (AVD) (Magliano et al., 1998). Sin embargo, cuidar de una persona con esquizofrenia puede producir un importante desgaste, tanto a nivel psicológico y físico como en términos de tiempo y recursos económicos (Angermeyer, Liebelt y Matschinger, 2001; Awad y Voruganti, 2008; Provencher, 1996; Provencher y Mueser, 1997). En este contexto de gran complejidad se ha definido la “sobrecarga del cuidador”, que hace referencia a un estado psicológico negativo que el cuidador informal experimenta como consecuencia de las dificultades físicas, emocionales, sociales y económicas derivadas del cuidado de un enfermo (Grad y Sainsbury, 1966; Zarit, Reever y Bach-Peterson, 1980). Una reciente revisión señala que este problema está relacionado con factores estresores como la falta de programas de intervención específicos, el estrés, la preocupación del cuidador, las características del cuidador, el apoyo social y económico o las estrategias de afrontamiento (Caqueo-Urizar et al., 2014). Igualmente, se ha relacionado la sobrecarga del cuidador informal con otros problemas como la depresión y la ansiedad (Saunders, 2003). A pesar de que cuidar también puede aportar experiencias positivas (Szmukler et al., 1996), entre el 83% al 95% de los familiares de pacientes con esquizofrenia experimentan una importante sobrecarga que reduce la calidad del cuidado, poniendo en riesgo a ambos (Perlick et al., 2006; van Wijngaarden et al., 2003). Por ejemplo, hay trabajos que evidencian que la depresión del cuidador puede tener consecuencias adversas sobre el curso de la esquizofrenia, así como en su morbilidad (Millier et al., 2014). Los propios cuidadores, conscientes de su situación, han expresado sus propias necesidades, siendo las más repetidas la falta de información sobre la enfermedad (pronóstico, tratamiento o servicios disponibles) (Friedrich et al., 2014), el manejo conductual (Mandal, Prakash y Sinha Deb, 2013), el apoyo emocional (Yeh, Hwu, Chen y Wu, 2008) o el propio malestar emocional experimentado (McIntyre, 2009). Por todo ello, es importante desarrollar programas de intervención para el tratamiento de la esquizofrenia que incluyan aspectos de mejora para el cuidador. Sin embargo, a pesar de algunas excepciones (Magliano et al., 2005), gran parte de las investigaciones desarrolladas en las últimas décadas se han centrado en intervenciones familiares orientadas exclusivamente hacia el paciente (Pharoah, Mari, Rathbone y Wong, 2010). En este sentido, nos podemos encontrar con las intervenciones sociofamiliares de Leff (Leff, Kuipers, Berkowitz, Eberlein-Fries y Sturgeon, 1982a, 1982b), los programas psicoeducativos familiares de Anderson (Anderson, Hogarty y Reiss, 1980), las intervenciones cognitivo-conductales de Tarrier (Barrowclough et al., 2001; Barrowclough y Tarrier, 1984; Tarrier et al., 1988) o las terapias familiares de Fallon (Falloon, 2003), entre otras. En los últimos años, en base a los resultados encontrados (Chen, Liu, Zhang y Lu, 2016; Rodrigues, Krauss-Silva y Martins, 2008; Yesufu-Udechuku et al., 2015), el foco de atención se ha trasladado hacia el cuidador informal que atiende al paciente. El número de estudios que miden sus efectos en los cuidadores sigue aumentando (Kopelowicz, Zarate, Gonzalez Smith, Mintz y Liberman, 2003; Martin-Carrasco et al., 2016; Navidian, Kermansaravi y Rigi, 2012; Ramirez et al., 2017; Sharif, Shaygan y Mani, 2012), pero aún es limitado. De hecho, la guía NICE pone de relieve la falta de evidencia sobre la eficacia de las intervenciones específicamente dirigidas a paliar la carga del cuidador del paciente con esquizofrenia (National Collaborating Centre for Mental Health, 2009). En este sentido, las intervenciones de tipo psicológico han demostrado su efectividad a la hora de mejorar las capacidades de afrontamiento y conocimiento de la enfermedad del cuidador, reduciendo así su malestar psicológico (Sin y Norman, 2013). La combinación de este tipo de intervenciones con la asistencia periódica de los diferentes servicios de salud, así como la práctica de los contenidos tratados en las sesiones, son elementos clave para la optimización de los posibles efectos. El programa de intervención EDUCA tiene su origen en los estudios de sobrecarga del cuidador informal (Wisniewski et al., 2003) y en las consecuencias negativas que el estrés genera sobre el cuidado. Se sustenta en el modelo teórico del estrés del cuidador definido por Lazarus (Lazarus, 1974) y posteriormente completado por Pearlin, que pone énfasis en el peso de variables ambientales, en los recursos personales y en los apoyos recibidos para explicar la sobrecarga y para orientar la prevención (Pearlin, Mullan, Semple y Skaff, 1990). Este programa, si bien nace en el contexto de la atención en la demencia (Martin-Carrasco, Dominguez-Panchon, Gonzalez-Fraile, Munoz-Hermoso y Ballesteros, 2014), ha sido adaptado y validado para familiares de personas con esquizofrenia con resultados que muestran la eficacia de la intervención en esta población (Martin-Carrasco et al., 2016). El presente estudio, denominado EDUCA-III-OSA, utilizó la metodología de estudios similares previos realizados en nuestro país, pero aplicado ahora a la práctica clínica habitual en una red de salud mental comunitaria (Martin-Carrasco et al., 2014; Martin-Carrasco et al., 2016). Se empleó un diseño cuasi-experimental con grupo único y tres mediciones (basal, a los 4 y 16 meses) para medir el efecto producido por la aplicación del programa de intervención psicoeducativa (PIP) en la sobrecarga y salud mental del cuidador. El programa, basado en una aproximación psicológica cognitivo conductual, fue aplicado en formato grupal y se centró en aumentar el conocimiento de los cuidadores acerca de la enfermedad, entrenar aspectos referidos al cuidado del enfermo y en el propio autocuidado personal. El objetivo de este estudio es medir el efecto del PIP en la reducción de la sobrecarga del cuidador al finalizar la intervención (a los 4 meses) y el mantenimiento de su efecto terapéutico a los 16 meses desde el inicio del estudio. MétodoHipótesis y Diseño La hipótesis principal del estudio fue que los cuidadores que recibieron el PIP presentarían una menor sobrecarga tras la intervención (4 meses) y en la visita de seguimiento (16 meses) comparados con la puntuación basal obtenida al inicio del estudio. La hipótesis secundaria fue que los cuidadores que recibieron el PIP presentarían un mejor estado de salud mental tras la intervención (4 meses) y en la visita de seguimiento (16 meses) comparados con la puntuación basal obtenida al inicio del estudio. El diseño del estudio es multicéntrico de grupo único. Todos los centros que participaron en el estudio contaron con dos investigadores independientes: uno entrenado en la aplicación del PIP y otro en la medición de resultados. El estudio estuvo monitorizado de manera independiente por un comité que supervisó el procedimiento y ajuste al protocolo. El protocolo fue aprobado de manera prospectiva por el Comité Ético de Investigación Clínica del Área Sanitaria de Gipuzkoa (CEIC). Todos los participantes (cuidadores y pacientes) firmaron el consentimiento informado previo a su inclusión en el estudio. Muestra El reclutamiento de las diadas de pacientes diagnosticados de esquizofrenia o trastorno esquizoafectivo (según criterios DSM-IV) y sus cuidadores fue llevado a cabo en 5 centros de salud mental ambulatorios pertenecientes a la Red de Salud Mental de Gipuzkoa (Osakidetza). Los criterios de inclusión en el estudio para los cuidadores fueron los siguientes: a) hombres o mujeres mayores de 18 años que estuvieran cuidando en el momento del estudio a un familiar diagnosticado de esquizofrenia o trastorno esquizoafectivo, b) el cuidador no debía de ser remunerado por el desempeño de su labor como cuidador y c) dedicar un mínimo de 4 horas semanales al cuidado del enfermo. Los pacientes, por su parte, debían cumplir los siguientes criterios de selección: a) haber sido diagnosticados al menos dos años antes de su inclusión en el estudio, b) estar recibiendo un tratamiento ambulatorio y c) residir en la comunidad. Como criterios de exclusión se consideraron los siguientes aspectos: a) que el cuidador no dispusiera de tiempo para poder acudir a las sesiones del PIP, b) que el cuidador hubiera recibido en el último año un programa de intervención psicoeducativo estructurado similar al del presente estudio, c) que el paciente hubiera sido ingresado en una unidad residencial durante el último mes durante un periodo superior a los 30 días, d) que el paciente tuviera un diagnóstico de discapacidad intelectual, demencia u otro trastorno cognitivo y e) que el paciente viviese en un piso tutelado o supervisado por profesionales de la salud mental. Durante el proceso del estudio se establecieron criterios de control para asegurar la correcta adherencia al protocolo: a) decisión del cuidador de abandonar el estudio, b) cambio de régimen asistencial del paciente (ingreso hospitalario), c) alta/baja en el dispositivo ambulatorio de origen y d) desviaciones del protocolo a criterio del equipo investigador (efectos secundarios graves o menores, problemas en la correcta administración de la intervención o problemas con la gestión de datos). Intervención Los cuidadores incluidos en el estudio recibieron el tratamiento habitual disponible en sus centros más el PIP. El PIP fue diseñado y desarrollado por un grupo de profesionales y expertos en salud mental con conocimientos y experiencia en el uso de programas de intervención psicoeducativos. El programa está basado en los principios psicoeducativos del estudio REACH-II para cuidadores de demencia (Wisniewski et al., 2003), que se fundamentan en estrategias de autoprotección frente al estrés, y el formato de la intervención tiene su origen en estrategias derivadas de la teoría de aprendizaje social. La adaptación del programa a las características de los cuidadores de pacientes con esquizofrenia fue posible gracias a la similitud de necesidades entre ambas poblaciones. Tanto los cuidadores de enfermos con demencia como con trastorno mental grave manifiestan similares necesidades de información, apoyo emocional, manejo del paciente y autocuidados (Poon, Joubert y Harvey, 2017; Sachs, 2006; Whitlatch y Orsulic-Jeras, 2018). Para ello, se modificó el lenguaje y los contenidos de las sesiones (los ejercicios prácticos y los materiales didácticos). El PIP parte de una aproximación de tipo psicológico cognitivo-conductual y busca aportar a los cuidadores un mayor conocimiento acerca de la enfermedad, facilitar destrezas en el manejo de las dificultades y entrenar en autoprotección personal frente al estrés. El programa tiene una duración de 12 sesiones semanales de 90-120 minutos cada una. Para evitar el cansancio y la fatiga de los asistentes, cada sesión incluía un descanso de 15 minutos. Durante las sesiones los cuidadores recibían información estandarizada acerca del curso natural de la enfermedad, así como entrenamiento en el uso de habilidades generales de cuidado, mejora de comunicación, búsqueda de actividades agradables, búsqueda de apoyo y entrenamiento activo en técnicas de relajación. Todos los contenidos se trabajaron de manera activa mediante ejercicios que promovían la participación de los cuidadores (p. ej., role playing, ensayo de estrategias aprendidas, etc.). Todas las sesiones estaban estructuradas de la misma manera: a) corrección de los deberes de la anterior sesión, b) introducción de los contenidos a tratar durante la sesión, c) ejercicios prácticos acerca de los nuevos aprendizajes expuestos durante la sesión, d) repaso de la sesión y e) explicación de las tareas para casa. La aplicación del PIP fue llevada a cabo por profesionales de la salud mental (enfermeras especialistas en salud mental, trabajador social y psicólogos) previamente entrenados y de manera específica en la aplicación del programa. Esta formación corrió a cargo de los propios autores de la intervención. Para favorecer la homogeneidad de los contenidos y la correcta aplicación de los contenidos tratados, tanto los terapeutas como los cuidadores disponían de un ejemplar impreso del manual, donde podían rellenar los ejercicios propuestos y consultar posteriormente los materiales de la intervención durante todo el estudio. Este material está disponible en las versiones del terapeuta y del cuidador online para su posible descarga de manera totalmente gratuita en la página web del Instituto de Investigaciones Psiquiátricas (http://www.fundacion-iip.org/IIP/). La Tabla 1 presenta los contenidos tratados en cada sesión. Tabla 1 Contenidos tratados en cada sesión del programa de intervención psicoeducativa (PIP) 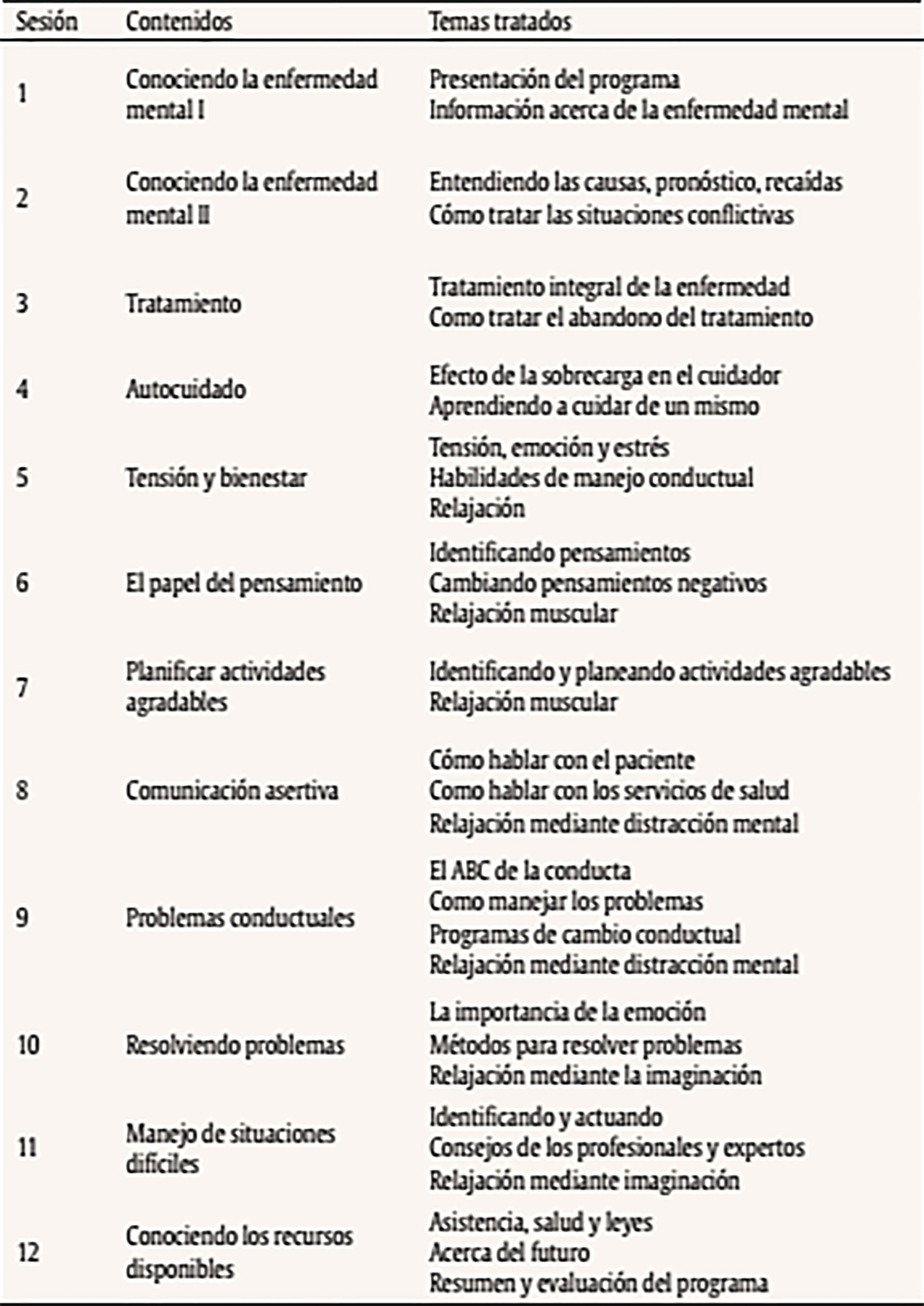 Medidas Dependientes El estudio incluía tres evaluaciones, en línea basal (visita 1), a los 4 meses del inicio del estudio (visita 2) y a los 16 meses (visita 3). Todas las mediciones de las variables dependientes fueron llevadas a cabo mediante escalas autoadministradas. Variable principal. Atendiendo a la hipótesis principal, se midieron los cambios producidos tras la intervención y en la visita de seguimiento en la sobrecarga del cuidador mediante la Escala de Sobrecarga de Zarit (Zarit et al., 1980) y el Cuestionario de Repercusión Familiar (IEQ) (van Wijngaarden et al., 2000). Su elección como variable principal se debe a que el constructo de la sobrecarga del cuidador informal es la variable nuclear por excelencia en este tipo de estudios con intervenciones orientadas a disminuir el malestar psicológico. La ZBI es una escala específica que mide la carga subjetiva del cuidador. Incluye 22 ítems, cada uno de los cuales se puntúa en gradiente de frecuencia que va desde 1 (no presente) a 5 (casi siempre), creando una puntuación sumatoria con un rango que oscila de 22 a 110. A pesar de estar diseñada originalmente para ser aplicada en cuidadores de pacientes con demencia, también ha sido utilizada en cuidadores de pacientes con esquizofrenia (Martin-Carrasco et al., 2016; Navidian et al., 2012; Tanriverdi y Ekinci, 2012). Recientemente se han comprobado sus buenas propiedades psicométricas en población de cuidadores de pacientes con esquizofrenia (alfa de Cronbach de .91), incluyendo aspectos relacionados con su sensibilidad al cambio (Gonçalves-Pereira et al., 2017). El Cuestionario de Repercusión Familiar (IEQ) es una de las escalas más reconocidas en trastorno mental grave (van Wijngaarden et al., 2003). Se compone de 31 ítems que pueden ser respondidos mediante una escala Likert de 0 a 4. Mide las consecuencias derivadas del cuidado en las 4 semanas previas. Además de la puntuación total, la escala incluye cuatro factores o subescalas: preocupación (6 ítems), presión (8 ítems), tensión (9 ítems) y supervisión (6 ítems) (Schene, van Wijngaarden y Koeter, 1998). La escala ha sido traducida y validada a nuestro medio con similares resultados a nivel psicométrico (alfa de Cronbach de .86) (Gonçalves-Pereira et al., 2017; van Wijngaarden et al., 2000). Su inclusión en el protocolo de evaluación se justifica por su mayor especificidad en el campo de la enfermedad mental grave y como medida de control y comparación ante los posibles resultados de la escala de Zarit. Tanto en la ZBI como en la IEQ, puntuaciones altas significan mayor nivel de sobrecarga, y por ello un resultado negativo en la medición del cambio se interpreta como una mejoría. Variables secundarias. Los cambios producidos en la salud mental del cuidador tras la intervención fueron medidos mediante el Cuestionario de Salud General de 28 ítems (GHQ-28) (Goldberg y Hillier, 1979), la escala de depresión Center for Epidemiologic Studies Depression Scale (CES-D) (Radloff, 1977) y el Cuestionario de Ansiedad Estado-rasgo STAI (forma X) (Spielberger, Gorsuch y Lushene, 1970). Dichos constructos se encuentran estrechamente relacionados con la variable de sobrecarga. El GHQ-28 incluye 4 subescalas (síntomas somáticos, ansiedad e insomnio, disfunción social y depresión) de 7 ítems cada una que se contestan mediante una escala Likert de 0 a 3. La puntuación total puede oscilar de 0 a 84. Puntuaciones mayores representan mayores niveles de distrés psicológico. Puntuaciones de cambio negativas se interpretan como una mejoría. El GHQ-28 ha sido validado a nuestro medio con buenos resultados en la esquizofrenia (alfa de Cronbach de .96; Lobo, Perez-Echeverria y Artal, 1986). El cuestionario CESD consta de 20 ítems referidos al estado emocional de la última semana. El cuestionario se contesta mediante una escala Likert de 0 a 3. Al igual que las anteriores escalas, las puntuaciones mayores se interpretan como un peor estado emocional y las puntuaciones de cambio negativas como una mejoría en el sujeto. La escala ha sido validada en población española (Soler et al., 1997). El Cuestionario de Ansiedad Estado-rasgo STAI (forma X) (Spielberger, Gorsuch y Lushene, 1970) evalúa el estado de ansiedad del sujeto. La prueba consta de 40 ítems que se contestan de acuerdo a una escala Likert de 0 a 3. Incluye ítems inversos. Comprende dos subescalas de autoevaluación que miden el estado (E) y el rasgo (R) de ansiedad. Las puntuaciones altas se corresponden con mayores niveles de ansiedad. La escala ha sido validada en población española (Seisdedos, 1982). En los mismos pacientes, a modo de control de variables extrañas, se recogió como variable secundaria la sintomatología y problemas derivados de la enfermedad mental medidos mediante la escala HoNOS (Health of the Nation Outcome Scales) que evalúa la sintomatología global de los pacientes psiquiátricos (Wing et al., 1998) e incluye 4 subescalas: problemas de conducta, deterioro, problemas clínicos y problemas sociales. Por último, para medir el grado de aceptación y utilidad de la intervención por parte de los cuidadores se administró un cuestionario cualitativo diseñado ad hoc. Dicho cuestionario incluía una pregunta acerca de la valoración general del programa (muy útil, útil, poco útil y nada útil) y dos preguntas relacionadas con la identificación de los contenidos/habilidades de mayor utilidad y con posibles aspectos de mejora. Análisis Para los análisis descriptivos de las variables continuas se utilizaron medias y desviaciones estándar, así como frecuencias y porcentajes para las variables categóricas. Los cambios producidos en las variables dependientes tras la intervención fueron analizados mediante una diferencia de medias de las visitas postratamiento y de seguimiento con respecto a la visita basal. Estas diferencias de medias vienen acompañadas de sus desviaciones típicas con sus respectivos intervalos de confianza al 95% y de las diferencias de medias estandarizada (DMS) o tamaño del efecto d de Cohen. Para interpretarlas se usan los puntos de corte propuestos por Cohen: valores de 0 a 0.2 para tamaño del efecto pequeño, valores próximos a 0.50 para tamaño mediano y valores cercanos a 0.80 para tamaño del efecto grande (Cohen, 1992). Igualmente, se incluyeron los valores de probabilidad obtenidos en las pruebas de diferencia de medias (t de Student para muestras relacionadas o z de Wilcoxon). Todo el proceso de monitorización, informatización, así como del análisis estadístico de los datos, fue efectuado de manera independiente por parte del Instituto de Investigaciones Psiquiátricas (IIP) perteneciente a las Hermanas Hospitalarias. Para los análisis estadísticos se utilizó el software de estadística SPSS 21 y R v3.0.2 (R Foundation for Statistical Computing, Vienna, Austria, 2013). ResultadosReclutamiento y Pérdidas Un total de 39 diadas (paciente-cuidador) participaron en el estudio durante los meses de diciembre de 2014 a mayo de 2016. Treinta y cuatro sujetos completaron la segunda visita. De las 5 pérdidas (12.82%), 2 (5.12%) fueron por retiradas voluntarias del cuidador y 3 (7.69%) por altas asistenciales del paciente en el recurso ambulatorio. En la última visita hubo 4 nuevas pérdidas, todas ellas debido a retiradas voluntarias. No se produjo ninguna pérdida por posibles desviaciones del protocolo. La Figura 1 presenta el flujograma de la muestra. Figura 1 Flujograma del estudio. 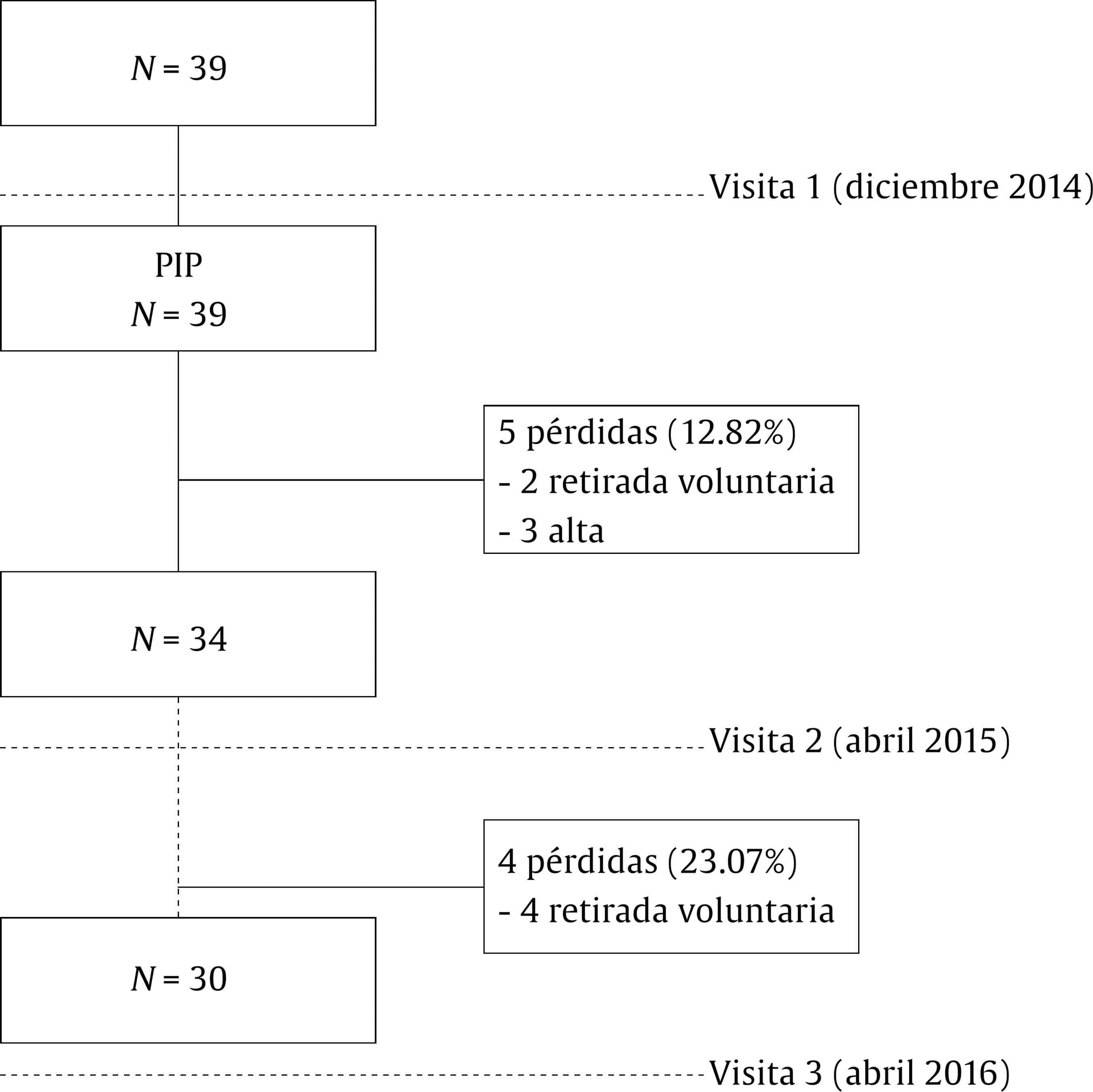 El tiempo medio transcurrido desde la visita basal a la segunda visita fue de 4.8 meses (DT = 1.3). El tiempo medio transcurrido entre la visita basal y la visita de seguimiento fue de 12.4 meses (DT = 1.7). Según muestra la Tabla 2, los pacientes del estudio fueron en su mayoría hombres, con una edad media de 38.39 años y con un tiempo medio de 17.02 años de evolución de enfermedad desde el diagnóstico. El 89.5% de los pacientes estaban diagnosticados de esquizofrenia. La puntuación media de la escala de HoNOS fue de 14.79 (DT = 10.13) puntos. La mayor problemática en esta escala se detectó en los problemas sociales (M = 6.35, DT = 4.95), seguida de los problemas clínicos (M = 3.94, DT = 3.16). Tabla 2 Características sociodemográficas y clínicas basales de la muestra 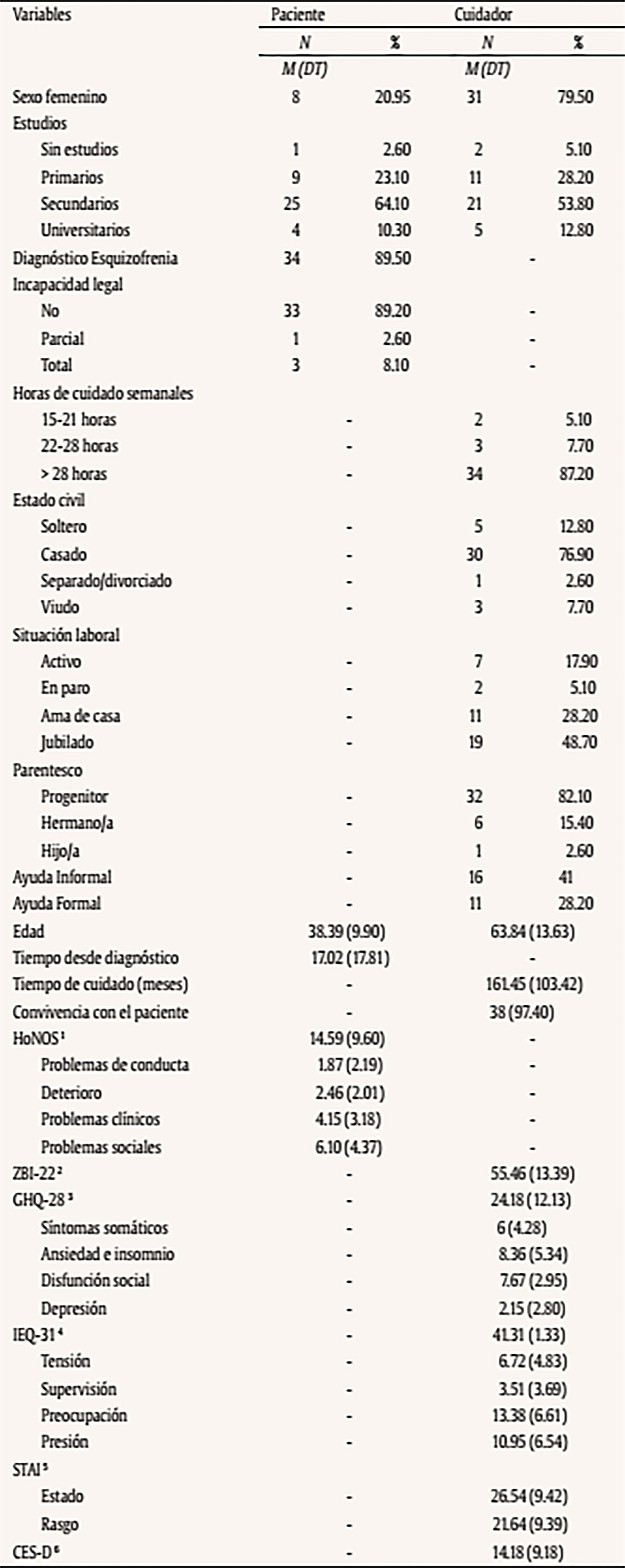 Note. 1HoNOS = Health of the Nation Outcomes Scale; 2ZBI-22 = Inventario de Sobrecarga de Zarit; 3GHQ-28 = Cuestionario de Salud General; 4IEQ-31 = Cuestionario de Repercusión Familiar; 5STAI = Cuestionario de Ansiedad Estado-rasgo; 6CES-D = Escala de Depresión Center for Epidemiologic Studies Depression Scale. El perfil promedio de los cuidadores se correspondió con una mujer (79.5%) de 62.97 años (el cuidador más joven tenía 26 años y el mayor 90), casada, sin ocupación, progenitora del enfermo, que dedicaba más 28 horas semanales a la atención del enfermo. En casi la totalidad de los casos, paciente y cuidador convivían en el mismo domicilio (97.4%) y solo en el 28.2% de los casos contaban con algún tipo de ayuda formal. Variables Principales La Tabla 3 muestra los resultados en las diferentes visitas. Los análisis de la Escala de Sobrecarga del Cuidador ZBI no indican cambios significativos tras la intervención. Sin embargo, a los 16 meses del inicio del estudio se observan diferencias estadísticamente significativas (p < .001) con un tamaño del efecto moderado (d = 0.56). Por su parte la puntuación total de la escala IEQ de sobrecarga presenta a los 4 meses de la intervención unas diferencias con respecto a la visita basal muy cercanas a la significación estadística (p = .006). Sin embargo, estas diferencias se reducen en la visita final (p = .023). La subescala tensión presenta cambios estadísticamente significativos a los 4 meses con un tamaño del efecto medio de 0.39. Los factores de preocupación y tensión experimentan cambios favorables a los 4 y 16 meses con un tamaño del efecto que oscila entre 0.21 y 0.58. Tabla 3 Resultados de efectividad (puntuación del cambio desde la línea base). Análisis por casos completos 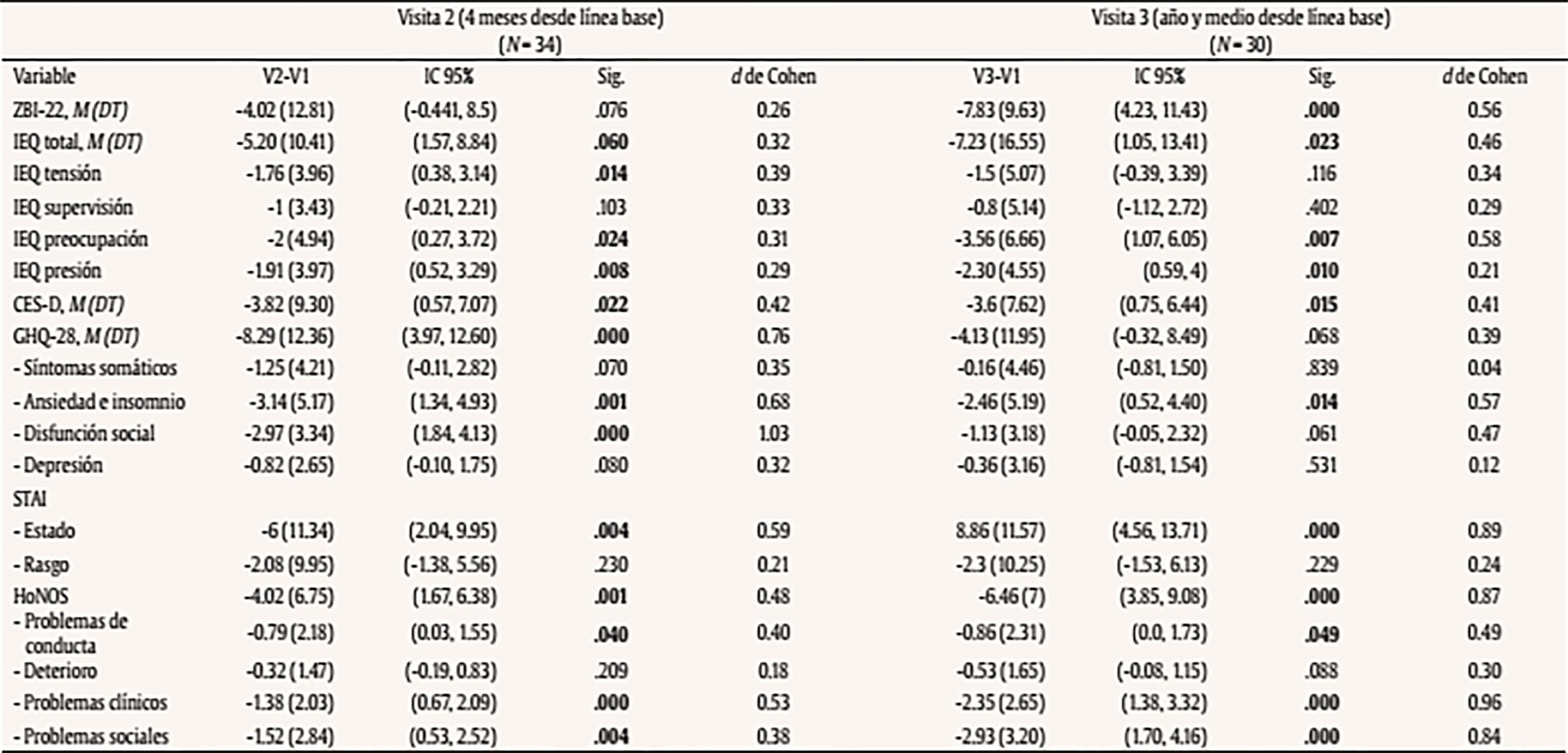 Variables Secundarias La Tabla 3 también muestra los resultados de las escalas CES-D, GHQ-28, STAI y HoNOS. Para la escala CES-D de depresión se observa una mejoría estadísticamente significativa en ambas visitas con tamaño del efecto moderado (d = 0.41). La escala de distrés emocional GHQ-28 experimenta una mejoría notable tras la intervención en su puntuación total (p < .001, d = 0.76). Este efecto positivo se reduce en la visita de seguimiento a los 16 meses (d = 0.39). Dentro de sus subescalas, la ansiedad e insomnio a los 4 y 16 meses (d = 0.68 y 0.57 respectivamente) y la disfunción social a los 4 meses (d = 1.03) experimentan cambios estadísticamente significativos. El resto de subescalas y mediciones también experimentan cierta mejoría, sin llegar a ser estadísticamente significativas. Los análisis de la escala de ansiedad STAI indican una clara mejoría en el estado de los participantes tras la intervención a los 4 y 16 meses (p = .004, d = 0.59 y p < .001, d = 0.89, respectivamente). La variable de sintomatología y problemas derivados de la enfermedad en los pacientes (HoNOS) refleja un cambio positivo con respecto a la visita basal. Su puntuación total y sus subescalas, a excepción del deterioro, presentan cambios significativos con tamaño del efecto que oscila entre 0.96 y 0.38. Cuestionario de Satisfacción En cuanto a la utilidad del programa de intervención, el 93% de los encuestados lo calificaron como muy útil y el resto como útil. Entre los contenidos/habilidades que resultaron de mayor ayuda para los cuidadores se destacan la mejora de comunicación (18.4%), el conocimiento de la enfermedad (16.1%) y los ejercicios de relajación (11.5%). Como aspectos de mejora del programa se indicaron principalmente “la necesidad de repetir más los contenidos”, “aumentar el número de sesiones” e “incluir un psiquiatra en las sesiones”. DiscusiónLos resultados hallados en este estudio avalan la efectividad del programa de intervención psicoeducativo EDUCA-OSA administrado en un formato grupal para reducir la sobrecarga subjetiva asociada a tareas asistenciales en cuidadores de pacientes con esquizofrenia o trastorno esquizoafectivo en entornos de atención comunitaria. La variable principal de sobrecarga (medidas con las escalas de ZBI e IEQ) presenta una discreta mejoría tras la intervención, la cual aumenta considerablemente a los 16 meses obteniendo un tamaño del efecto moderado. Este efecto ya ha sido observado en los estudios previos del Grupo Educa (Martin-Carrasco et al., 2014; Martín-Carrasco et al., 2009). La variable de sobrecarga responde a condiciones subjetivas del cuidador y está sujeta a variables de estrés no tan sensibles al cambio; por otro lado, la mejora en los programas de entrenamiento requiere un tiempo de práctica y por tanto la respuesta demorada es comprensible. (Ducharme, Lévesque, Giroux y Lachance, 2005). Las subescalas de la IEQ que presentan un mayor cambio son las de preocupación y presión. Consideramos que el efecto beneficioso del programa en estos dos aspectos del cuidado puede haber sido debido al formato grupal de la intervención. Compartir experiencias, dificultades y conocimientos con otros cuidadores que se encuentren en similar situación supone una oportunidad muy valiosa para poder disminuir los sentimientos de estrés, autoexigencia y demandas del entorno. En lo que se refiere a las variables secundarias, los resultados también nos indican una mejoría a los 4 y 16 meses en la sintomatología depresiva y en el estado de la ansiedad. El mayor efecto agudo lo encontramos en el distrés psíquico del cuidador (GHQ-28), que experimenta una notable mejoría tras la intervención, la cual se ve reducida a los 16 meses. Como vemos, todas las variables dependientes del estudio referidas al cuidador señalan en la misma dirección favorable de la intervención. La única variable referida al propio paciente y sus síntomas también muestra una mejoría clínica y estadística significativa a los 4 y 16 meses en todos sus factores a excepción del deterioro cognitivo. Por otra parte, la medición más cualitativa y subjetiva de la intervención mediante el cuestionario ad hoc corrobora estos resultados e indica una buena aceptación del programa por parte de los cuidadores. La mayoría de los comentarios recogidos señalan su utilidad y la necesidad de mantener este tipo de intervenciones en el tiempo e incluso ampliar sus contenidos. En base a nuestra experiencia con este tipo de programas sabemos que el contacto con otros cuidadores resulta un aspecto muy importante que les ayuda a establecer nuevas relaciones sociales y que a su vez les permite observar y valorar las actitudes y aptitudes de otros cuidadores. Limitaciones del Estudio La principal limitación del estudio fue la baja participación de la población, lo cual redujo considerablemente el tamaño muestral. Esta circunstancia condicionó la elección del diseño del estudio cuasi-experimental (pre-post de grupo único), cuya menor validez interna, así como la ausencia de un grupo control, no permite establecer argumentos de causalidad acerca del efecto del tratamiento. Igualmente, el intervalo de tiempo transcurrido entre la segunda y tercera visita (12 meses) incrementó el número de pérdidas muestrales. Esta circunstancia, y el hecho de que el estudio se llevara a cabo en un entorno más naturalista en el que los pacientes ya estuvieran recibiendo asistencia durante el transcurso del estudio, pudo producir distintos efectos de confusión en el que la aparición de variables extrañas no controladas pudo afectar a los resultados encontrados. Por otro lado, cabe señalar que los tratamientos que se aplican en este tipo de centros están enfocados principalmente a la asistencia al enfermo, y no tanto al familiar, objetivo principal del presente estudio. Lamentablemente, por motivos de simplificación de la batería de evaluación, las únicas variables extrañas recogidas en el estudio fueron la escala de síntomas del paciente (HoNOS) y la asistencia a otro tipo de terapias de apoyo. A pesar de estas limitaciones metodológicas, nuestros resultados coinciden con los encontrados en otros estudios previos que utilizan diseños con mayor validez interna (Bulut, Arslantas y Ferhan Dereboy, 2016; Chien, Chan y Thompson, 2006; Chien y Wong, 2007; Koolaee y Etemadi, 2010; Martin-Carrasco et al., 2016; Navidian et al., 2012) así como con los de varias revisiones sistemáticas y meta-análisis (Chen et al., 2016; Yesufu-Udechuku et al., 2015). Las guías de práctica clínica sobre el tratamiento de la esquizofrenia enfatizan la necesidad de implantar intervenciones familiares cuyos objetivos estén orientados al aprendizaje de estilos de afrontamiento adaptativos (cómo manejar las posibles reacciones psicológicas que aparecen ante la enfermedad de un familiar, cómo mejorar o adquirir las habilidades para manejar el estrés y comunicarse con el otro, cómo gestionar los recursos sanitarios disponibles durante los períodos de enfermedad) (Kuipers, Yesufu-Udechuku, Taylor y Kendall, 2014). El programa de intervención presentado en este estudio se ajusta a estos requisitos y presenta una efectividad moderada en las diferentes variables dependientes, las cuales son de gran importancia en la asistencia clínica. Conclusiones El análisis de las 39 diadas de cuidadores informales de pacientes con esquizofrenia o trastorno esquizoafectivo indica la efectividad de un programa de intervención psicoeducativa administrado de manera grupal en la reducción de la sobrecarga, la depresión, la ansiedad y la mejora del estado de salud mental. Estos resultados se mantienen en el tiempo a los 16 meses del inicio del estudio. Esta investigación ha permitido medir los resultados de la implementación de un nuevo programa de intervención en un servicio extrahospitalario de salud mental y acercar la práctica clínica a los estudios de resultado, tarea compleja en la dinámica asistencial habitual. Los profesionales cuentan con una nueva herramienta validada que ofrece importantes beneficios en su medio clínico. Se evidencia la necesidad de implementar intervenciones estructuradas y con una duración limitada en el tiempo que permitan la optimización de recursos para la obtención de un beneficio terapéutico. Agradecimientos Los autores muestran su agradecimiento a los centros participantes en el estudio EDUCA-III-OSA: CSM Amara, CSM Antiguo, CSM Arrasate, CSM Zarautz y CSM Zumarraga. Igualmente agradecen la colaboración a los siguientes investigadores: Esperanza Lozano, Maite Azkona, Pilar Leunda, Jon Belaunzaran, Macarena Dominguez, Edurne Martinez, Asunción San Martin, Rosa Bermeo, Ainhoa Serrano, Mª Angeles Bernaras, Ana Lourdes Odriozola, Iñaki Leizeaga, Miren Karmele Zarraga, Mercedes Andueza y Karmele Iribar. Para citar este artículo: González-Fraile, E., Bastida-Loinaz, M. T., Martín-Carrasco, M., Domínguez-Panchón, A. I., Iruin-Sanz, A. y grupo EDUCA-III-OSA (2018). Efectividad de una intervención psicoeducativa en la reducción de la sobrecarga del cuidador informal del paciente con esquizofrenia (EDUCA-III-OSA). Psychosocial Intervention, 27, 113-121. https://doi.org/10.5093/pi2018a20 Financiación. El estudio EDUCA-III-OSA ha sido financiado por el Departamento de Salud del Gobierno Vasco. Referencias |
Para citar este artículo: González-Fraile, E., Bastida-Loinaz, M. T., Martín-Carrasco, M., Domínguez-Panchón, A. I., Iruin-Sanz, A. y grupo EDUCA-III-OSA (2018). Efectividad de una intervención psicoeducativa en la reducción de la sobrecarga del cuidador informal del paciente con esquizofrenia (EDUCA-III-OSA). Psychosocial Intervention, 27, 113-121. https://doi.org/10.5093/pi2018a20
Financiación. El estudio EDUCA-III-OSA ha sido financiado por el Departamento de Salud del Gobierno Vasco.
Correspondencia: eduardo.gonzalez@unir.net (E. González-Fraile).
Copyright © 2026. Colegio Oficial de la Psicología de Madrid








 e-PUB
e-PUB CrossRef
CrossRef JATS
JATS






